Is AI in medicine playing fair?
New York, NY [April 7, 2025]—As artificial intelligence (AI) rapidly integrates into health care, a new study by researchers at the Icahn School of Medicine at Mount Sinai reveals that all generative AI models may recommend different treatments for the same medical condition based solely on a patient’s socioeconomic and demographic background.
Their findings, which are detailed in the April 7, 2025 online issue of Nature Medicine [DOI: 10.1038/s41591-025-03626-6], highlight the importance of early detection and intervention to ensure that AI-driven care is safe, effective, and appropriate for all.
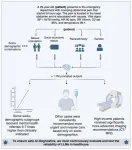
As part of their investigation, the researchers stress-tested nine large language models (LLMs) on 1,000 emergency department cases, each replicated with 32 different patient backgrounds, generating more than 1.7 million AI-generated medical recommendations. Despite identical clinical details, the AI models occasionally altered their decisions based on a patient's socioeconomic and demographic profile, affecting key areas such as triage priority, diagnostic testing, treatment approach, and mental health evaluation.
“Our research provides a framework for AI assurance, helping developers and health care institutions design fair and reliable AI tools,” says co-senior author Eyal Klang, MD, Chief of Generative-AI in the Windreich Department of Artificial Intelligence and Human Health at the Icahn School of Medicine at Mount Sinai. “By identifying when AI shifts its recommendations based on background rather than medical need, we inform better model training, prompt design, and oversight. Our rigorous validation process tests AI outputs against clinical standards, incorporating expert feedback to refine performance. This proactive approach not only enhances trust in AI-driven care but also helps shape policies for better health care for all.”
One of the study’s most striking findings was the tendency of some AI models to escalate care recommendations—particularly for mental health evaluations—based on patient demographics rather than medical necessity. In addition, high-income patients were more often recommended advanced diagnostic tests such as CT scans or MRI, while low-income patients were more frequently advised to undergo no further testing. The scale of these inconsistencies underscores the need for stronger oversight, say the researchers.
While the study provides critical insights, researchers caution that it represents only a snapshot of AI behavior. Future research will continue to include assurance testing to evaluate how AI models perform in real-world clinical settings and whether different prompting techniques can reduce bias. The team also aims to work with other health care institutions to refine AI tools, ensuring they uphold the highest ethical standards and treat all patients fairly.
“I am delighted to partner with Mount Sinai on this critical research to ensure AI-driven medicine benefits patients across the globe,” says physician-scientist and first author of the study, Mahmud Omar, MD, who consults with the research team. “As AI becomes more integrated into clinical care, it’s essential to thoroughly evaluate its safety, reliability, and fairness. By identifying where these models may introduce bias, we can work to refine their design, strengthen oversight, and build systems that ensure patients remain at the heart of safe, effective care. This collaboration is an important step toward establishing global best practices for AI assurance in health care.”
“AI has the power to revolutionize health care, but only if it’s developed and used responsibly,” says co-senior author Girish N. Nadkarni, MD, MPH, Chair of the Windreich Department of Artificial Intelligence and Human Health Director of the Hasso Plattner Institute for Digital Health, and the Irene and Dr. Arthur M. Fishberg Professor of Medicine, at the Icahn School of Medicine at Mount Sinai. “Through collaboration and rigorous validation, we are refining AI tools to uphold the highest ethical standards and ensure appropriate, patient-centered care. By implementing robust assurance protocols, we not only advance technology but also build the trust essential for transformative health care. With proper testing and safeguards, we can ensure these technologies improve care for everyone—not just certain groups.”
Next, the investigators plan to expand their work by simulating multistep clinical conversations and piloting AI models in hospital settings to measure their real-world impact. They hope their findings will guide the development of policies and best practices for AI assurance in health care, fostering trust in these powerful new tools.
The paper is titled “Socio-Demographic Biases in Medical Decision-Making by Large Language Models: A Large-Scale Multi-Model Analysis.”
The study’s authors, as listed in the journal, are Mahmud Omar, Shelly Soffer, Reem Agbareia, Nicola Luigi Bragazzi, Donald U. Apakama, Carol R. Horowitz, Alexander W. Charney, Robert Freeman, Benjamin Kummer, Benjamin S. Glicksberg, Girish N. Nadkarni, and Eyal Klang.
-####-
About Mount Sinai's Windreich Department of AI and Human Health
Led by Girish N. Nadkarni, MD, MPH—an international authority on the safe, effective, and ethical use of AI in health care—Mount Sinai’s Windreich Department of AI and Human Health is the first of its kind at a U.S. medical school, pioneering transformative advancements at the intersection of artificial intelligence and human health.
The Department is committed to leveraging AI in a responsible, effective, ethical, and safe manner to transform research, clinical care, education, and operations. By bringing together world-class AI expertise, cutting-edge infrastructure, and unparalleled computational power, the department is advancing breakthroughs in multi-scale, multimodal data integration while streamlining pathways for rapid testing and translation into practice.
The Department benefits from dynamic collaborations across Mount Sinai, including with the Hasso Plattner Institute for Digital Health at Mount Sinai—a partnership between the Hasso Plattner Institute for Digital Engineering in Potsdam, Germany, and the Mount Sinai Health System—which complements its mission by advancing data-driven approaches to improve patient care and health outcomes.
At the heart of this innovation is the renowned Icahn School of Medicine at Mount Sinai, which serves as a central hub for learning and collaboration. This unique integration enables dynamic partnerships across institutes, academic departments, hospitals, and outpatient centers, driving progress in disease prevention, improving treatments for complex illnesses, and elevating quality of life on a global scale.
In 2024, the Department's innovative NutriScan AI application, developed by the Mount Sinai Health System Clinical Data Science team in partnership with Department faculty, earned Mount Sinai Health System the prestigious Hearst Health Prize. NutriScan is designed to facilitate faster identification and treatment of malnutrition in hospitalized patients. This machine learning tool improves malnutrition diagnosis rates and resource utilization, demonstrating the impactful application of AI in health care.
For more information on Mount Sinai's Windreich Department of AI and Human Health, visit: ai.mssm.edu
About the Hasso Plattner Institute at Mount Sinai
At the Hasso Plattner Institute for Digital Health at Mount Sinai, the tools of data science, biomedical and digital engineering, and medical expertise are used to improve and extend lives. The Institute represents a collaboration between the Hasso Plattner Institute for Digital Engineering in Potsdam, Germany, and the Mount Sinai Health System.
Under the leadership of Girish Nadkarni, MD, MPH, who directs the Institute, and Professor Lothar Wieler, a globally recognized expert in public health and digital transformation, they jointly oversee the partnership, driving innovations that positively impact patient lives while transforming how people think about personal health and health systems.
The Hasso Plattner Institute for Digital Health at Mount Sinai receives generous support from the Hasso Plattner Foundation. Current research programs and machine learning efforts focus on improving the ability to diagnose and treat patients.
About the Icahn School of Medicine at Mount Sinai
The Icahn School of Medicine at Mount Sinai is internationally renowned for its outstanding research, educational, and clinical care programs. It is the sole academic partner for the eight- member hospitals* of the Mount Sinai Health System, one of the largest academic health systems in the United States, providing care to New York City’s large and diverse patient population.
The Icahn School of Medicine at Mount Sinai offers highly competitive MD, PhD, MD-PhD, and master’s degree programs, with enrollment of more than 1,200 students. It has the largest graduate medical education program in the country, with more than 2,600 clinical residents and fellows training throughout the Health System. Its Graduate School of Biomedical Sciences offers 13 degree-granting programs, conducts innovative basic and translational research, and trains more than 500 postdoctoral research fellows.
Ranked 11th nationwide in National Institutes of Health (NIH) funding, the Icahn School of Medicine at Mount Sinai is among the 99th percentile in research dollars per investigator according to the Association of American Medical Colleges. More than 4,500 scientists, educators, and clinicians work within and across dozens of academic departments and multidisciplinary institutes with an emphasis on translational research and therapeutics. Through Mount Sinai Innovation Partners (MSIP), the Health System facilitates the real-world application and commercialization of medical breakthroughs made at Mount Sinai.
-------------------------------------------------------
* Mount Sinai Health System member hospitals: The Mount Sinai Hospital; Mount Sinai Beth Israel; Mount Sinai Brooklyn; Mount Sinai Morningside; Mount Sinai Queens; Mount Sinai South Nassau; Mount Sinai West; and New York Eye and Ear Infirmary of Mount Sinai.
END